Why Choose Us
Learn more about Good Shepherd Rehabilitation Hospital, a destination for recovery for stroke, brain injury, spinal cord injury and complex medical rehabilitation.
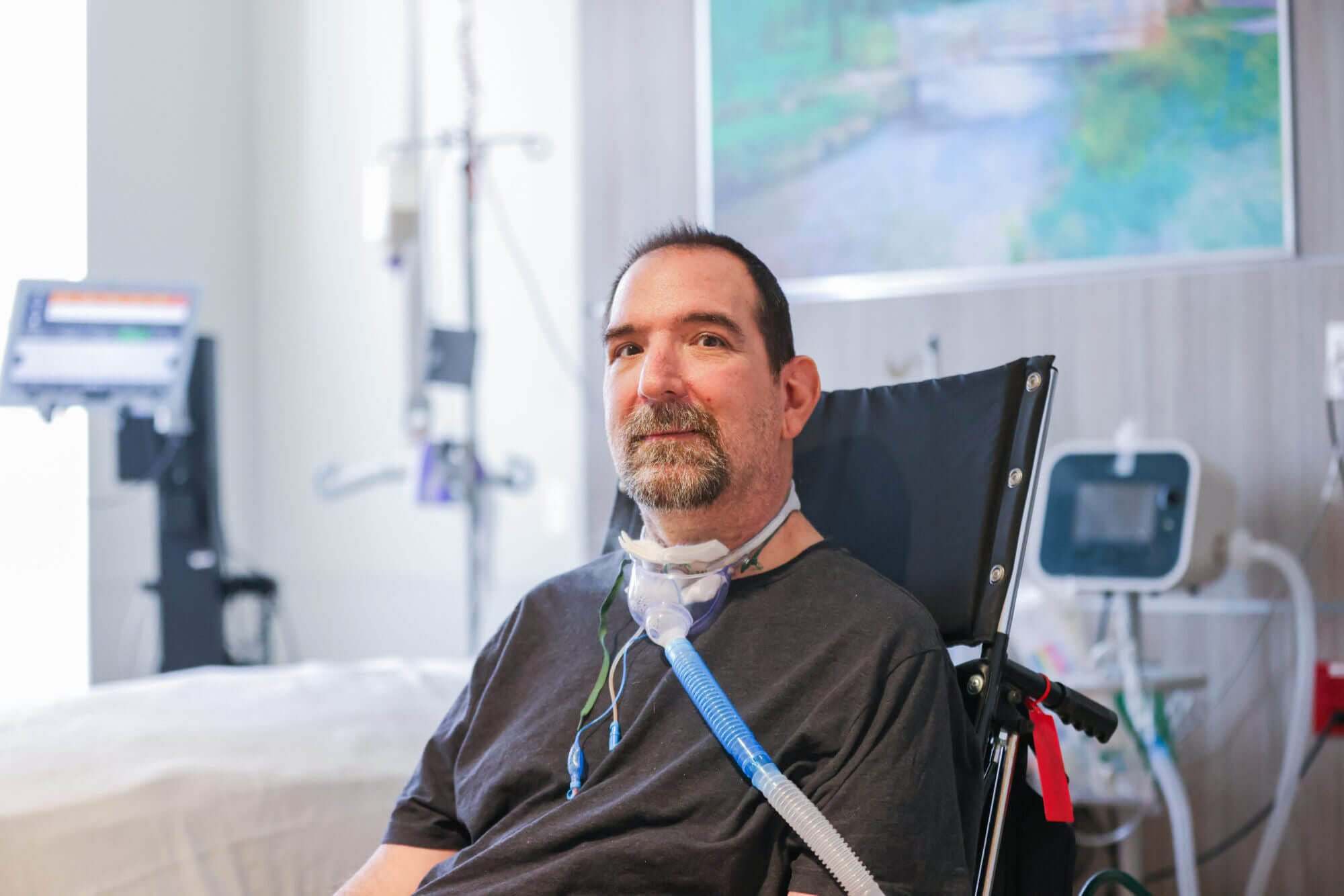
Drew Katona is a social, outgoing guy. His happiness and affable personality come through in his colorful language and stories. A woodworker by trade and an excellent cook by hobby, he could build you a custom dining table, then serve you a dinner on it with his homemade pesto.
But a year ago, Drew couldn’t talk. He couldn’t move. He couldn’t even open his eyes.
While traveling, he was hit by a sudden and severe onset of Guillain-Barré syndrome, a rare, incurable condition that wrecked his nervous system and completely paralyzed him.
He was hundreds of miles from home and his muscles had essentially turned to mush. His outgoing mind was still active, stuck inside his failing body.
“It was fun,” the 50-year-old quipped recently.
The lingering paralysis still affects his speech but hasn’t hurt his sense of humor. He’s still recovering, having relearned how to communicate and slowly regaining mobility — a journey that included five months at two Good Shepherd Rehabilitation hospitals. But those first weeks were difficult, full of snippets of memories and hallucinations. Even when he was aware of who or what was around him, he couldn’t interact.
“That is as hard as it sounds,” Drew said, momentarily serious. “It’s very difficult to be someone who is so outgoing and funny and talkative to anyone, to be on an island, so to speak. It was tough.”
Drew noticed something was off when he woke up the morning of Feb. 9, 2025, with a strange pins-and-needles feeling in his hands. A spreading tingling or weakness can be an early sign of Guillain-Barré syndrome, in which the body’s immune system attacks and damages the nerves, cutting off signals to and from the brain.
He went back to sleep.
“I kind of brushed it off until I stood up and almost fell down,” Drew said. “He was like Jell-O,” added Yvonne, his wife of 13 years.”
Drew and Yvonne were in New York’s Hudson Valley, back where they grew up to attend the funeral of a childhood friend later that day. They had flown up from their home in Wilmington, North Carolina, the night before and spent the evening out with loved ones.
Yvonne helped Drew to the bathroom, then back to the bed where they called her brother, a first responder. They thought it was a stroke, maybe a heart attack.
Within an hour Drew was in the emergency room, his condition quickly worsening. The doctor recognized Guillain-Barre and had him airlifted to another New York-area hospital for confirmation and treatment. Drew’s speech grew increasingly slurred. Yvonne sat with him through the night to make sure he kept breathing. By the next morning, doctors had him intubated, knowing the paralysis would get worse.
“That is the worst part,” Yvonne said. “That is the whole nature of Guillain-Barre: You’re there mentally, cognitively. It does not affect the brain at all. Drew was there. Anytime we would pause his medication drip, he would answer questions by moving his eyes. Every answer was right. He was perfectly aware, he was just locked in. That was really rough.”
Drew never made it to his friend’s service. He had thought, briefly, that maybe the ambulance could stop at the funeral home before he was airlifted. The friend’s family visited him later, during his rehabilitation.
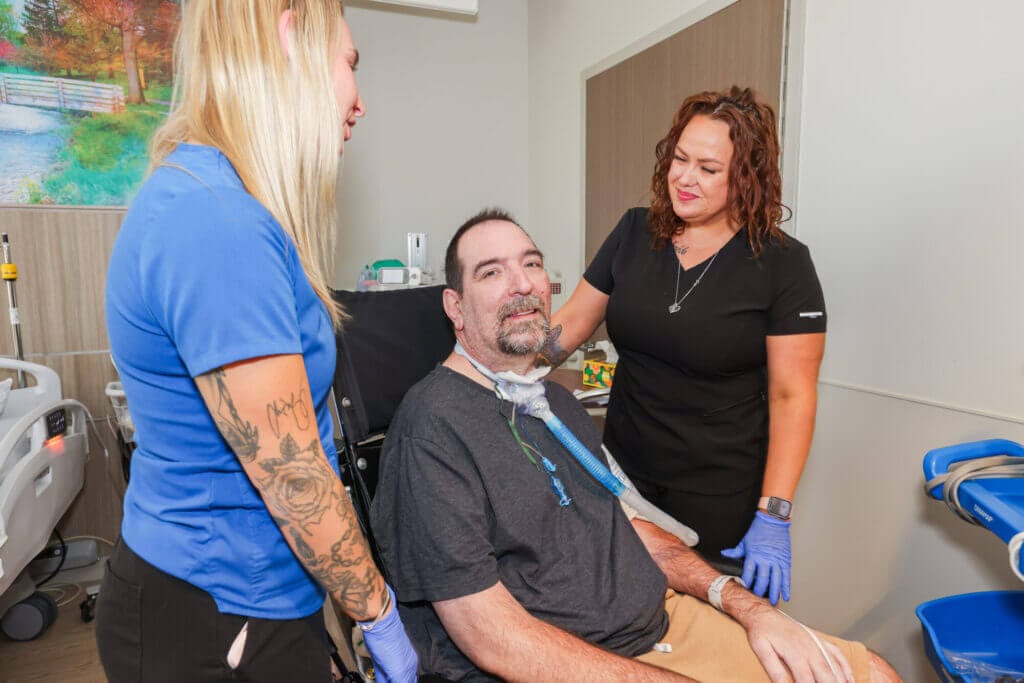
Drew’s early recovery is a blur in his memory, not just because he couldn’t see, but because the sedatives caused his conscious mind to fade in and out. It was difficult to tell what was real, what he really heard or what his drifting mind had simply made up.
“From the day that I was rushed into surgery for the intubation to the day that I was consciously aware of my surroundings was about two months. For me, it could have been a few days,” Drew said.
But he remembers his transfer by ambulance to the Lehigh Valley as the scariest part of his recovery. He had to be off medication for the roughly two-hour ride. His eyes were still closed, but without sedation, he was awake, aware and heard everything.
“I had no idea what … was going on,” he said. “Have I been stolen? I had no idea.”
He was headed to Good Shepherd’s long-term acute care hospital (LTACH) in Bethlehem: Good Shepherd Specialty Hospital. On their insurer’s recommendation, Yvonne had scouted Good Shepherd ahead of time and liked what she saw, especially patients’ private rooms and having the respiratory therapists close by. Drew ultimately came to agree.
“There is not a person that I encountered that was not amazing at that facility,” he said.
Drew spent the summer with Good Shepherd as he was weaned off the ventilator. By the end of June, he was transferred to Good Shepherd Rehabilitation Hospital in Center Valley, where he relearned how to talk.
“My goal is to walk back into the rehab up there and scare the … out of everyone again!”
Drew Katona
To that point, Yvonne had spoken for him. She stayed in a hotel nearby, visiting daily for Drew’s entire stay. Communication was incremental, starting with his eyes, then lip-reading.
As his mobility began to return, Drew was able to use a device called autonoMEgo, selecting options on a screen controlled by his eyes. This, Yvonne said, is where, after six months of paralysis, his personality and humor again began to shine through.
“He had a lot of fun with that machine,” she said of the autonoMEgo. “We made sure they cleared the history before we left!”
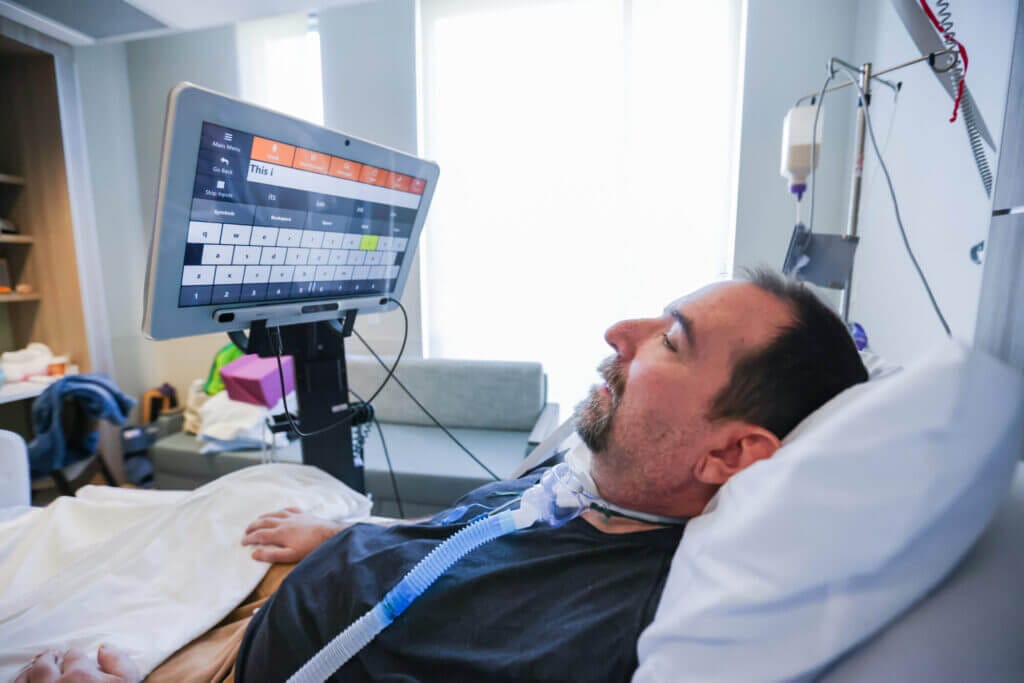
He continued to improve and around mid- to late August, Drew started speaking again, verbalizing multiple words at a time. It was a relief to Yvonne, knowing Drew could communicate his needs himself.
But Drew found a mischievous use for this rediscovered skill. Not everyone immediately knew he could talk. When an unsuspecting nurse entered the room, he would motion them over to the bed to touch his arm. Then Drew would scream.
“They would jump back, scared … because they didn’t know I could make a noise,” he laughed.
Yvonne quickly clarified: “Then they would start crying — with happiness!”
“That’s how I chose to use my newfound freedom, scaring … people,” Drew said.
Drew and Yvonne finally returned home at the end of September. They had planned on a two-day trip. They were gone eight months.
Back on the North Carolina coast, Drew continues with outpatient physical, occupational and speech therapies while working with a strength and conditioning coach and a visiting in-home therapist. Not only must he overcome severely damaged nerves but atrophied muscles, as well.
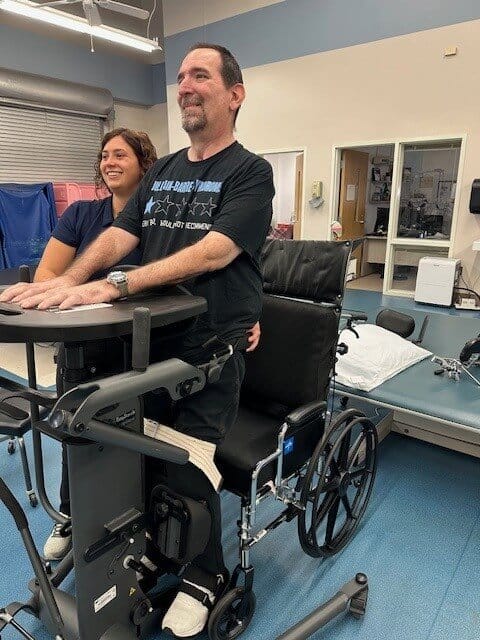
While there is no cure for Guillain-Barré, there is recovery. Drew takes inspiration from interviews he’s heard from patients like him who have lingering numbness or tingling, but no outward signs of illness. Recovery can take up to three years; a little over one year in, Drew figures he’s about halfway there.
“For me,” he said, “my prognosis is that I will be 100% or … near close to it by the end of all this. And that’s just going to take time. And I have to assume that I will be 100% until I’m told otherwise.”
There’s much to be done first. When Drew got home, he still couldn’t move his arms. Now, he can. He can also move his legs with machine assistance. That’s progress. He looks forward to the day he can walk in the backyard and feel grass between toes. Or drive a car. Or stand in the kitchen and cook again.
“You take nothing for granted after this,” not even the luxury of sitting at home and sipping from your own glass, Yvonne said.
Drew and Yvonne still have big plans. They want to travel to southern France and see the lavender fields in summer. They want to revisit Paris and Rome, their favorite cities.
Pennsylvania’s on the travel list, too.

“My goal is to walk back into the rehab up there and scare the … out of everyone again!” Drew yelled excitedly.
Yvonne again clarified, laughing: “We want to thank everyone up there.”
He just wants to do it in his own, outgoing way.
Photos: Ashli Truchon Novak and Katona Family